Breaking News
Popular News






Enter your email address below and subscribe to our newsletter

GLP-1 drugs cost $1,100–$1,400 per month. Novo Nordisk cut prices 35–50% in February 2026 after pressure from Congress and the Trump administration. Medicare negotiated $245/month. But for 22 million uninsured Americans and those on specialty insurance tiers? They’re paying full freight. These drugs work. They reduce cardiovascular death risk. They control obesity and diabetes. But for Millennials and Gen Z, a medication that could extend life is literally unaffordable. Billionaires take Ozempic for vanity. Working people ration doses or don’t fill the prescription at all.

Key Takeaways

Novo Nordisk, Eli Lilly, and Pfizer control the GLP-1 market. Prices before Feb 2026: Ozempic ($950–$1,100/month), Wegovy ($1,100–$1,300), Mounjaro ($1,200–$1,349), Zepbound ($1,400+). Manufacturing cost: $5–$10 per dose. List price: 110–280× manufacturing cost. Why so high?
Result: GLP-1s became the most profitable drug class in the world. Until Congress complained.
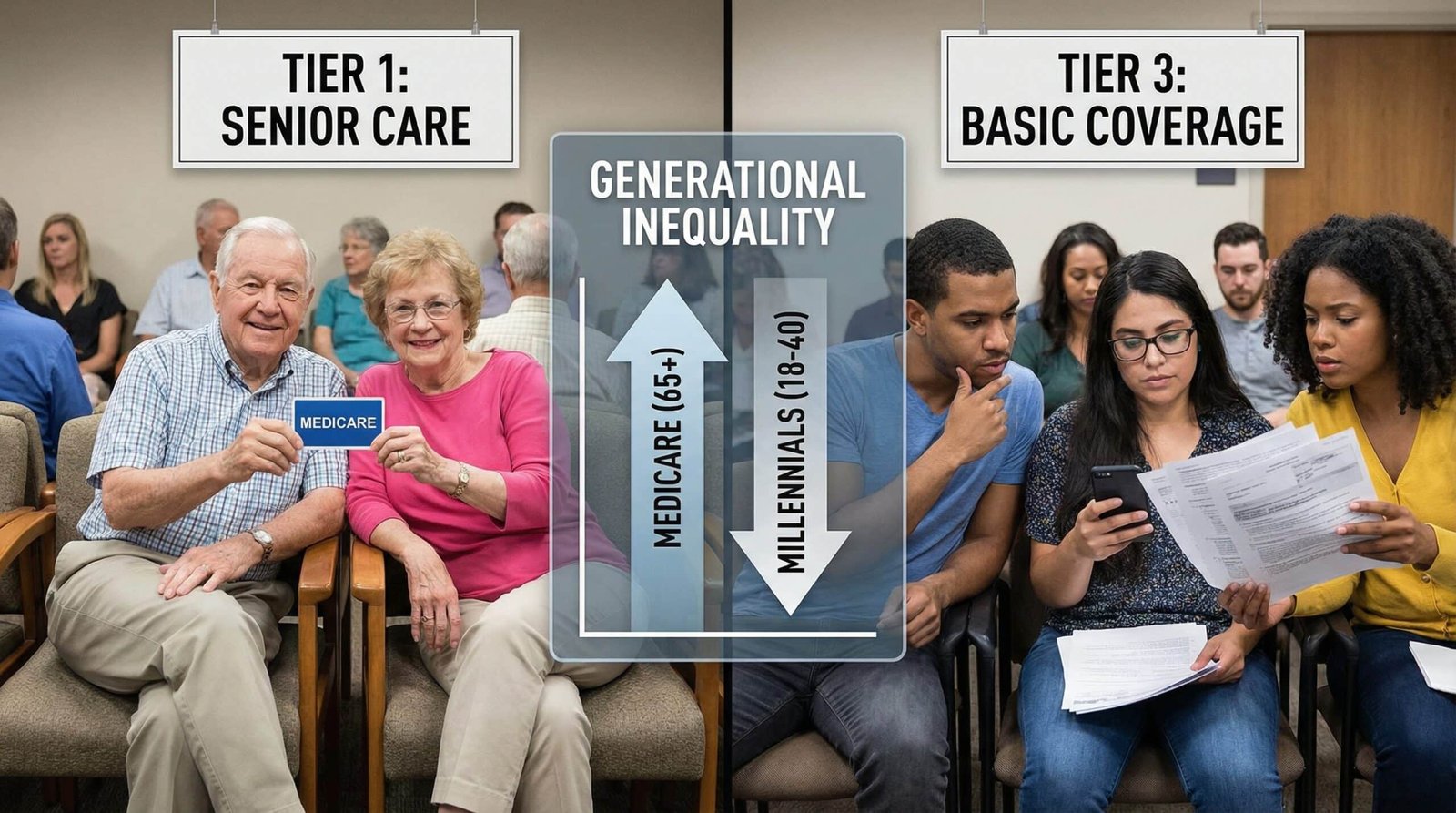
Medicare (65+): Negotiated $245/month (out-of-pocket $0–$50). Why? Seniors are a voting bloc. Congress gave Medicare statutory power to negotiate drug prices.
Commercial Insurance (younger workers): $150–$300/month in-network copay (requires prior authorization). Specialty tier: $300–$500. Insurance companies place GLP-1s on specialty tiers to drive high copays.
Uninsured (22 million Americans): List price $1,100–$1,400/month. Zero negotiating power. Pay full freight or go without.
Self-Insured (gig workers, freelancers): $1,100–$1,400/month without negotiation. Manufacturer savings programs sometimes reduce to $50–$300, but eligibility is complex.
Direct-to-Consumer (TrumpRx, Roman, GoodRx, Mark Cuban Cost Plus): $350/month for starter doses. Quality/oversight varies. No insurance required but no doctor oversight either.

On Feb 24, 2026, Novo Nordisk cut list prices 35–50%. Why the sudden generosity?
New list prices post-cut: ~$650–$700/month. But here’s the catch: Insurance copays stayed the same. Only uninsured patients benefit via manufacturer savings programs — maybe $50–$300 off. Still $400–$1,000+/month.
Truth: The cuts are PR. Insurance copays didn’t move. Medicare was already at $245. Uninsured patients saw minimal benefit.

On Apr 2, 2026 (today), Congress took a “fresh look at GLP-1 legislation on cost, safety.” They’re investigating:
Expect legislation by Q3 2026 capping copays at $50/month, mandating generic development, and limiting prior authorization. Manufacturers will lobby hard against it.

Boomer (70+ on Medicare): $245/month. Why? Seniors are a voting bloc. Congress prioritized Medicare drug negotiation.
Millennial (35–45, employer insurance): $150–$500/month, depending on tier placement. Good health plan? $150. Mediocre? $500.
Gen Z (25–35, no insurance or high-deductible plan): $1,100–$1,400/month. Cannot afford lifesaving drug.
The injustice: GLP-1s reduce cardiovascular death significantly. Younger people with chronic disease (diabetes, obesity) need lifelong treatment. At $1,400/month, that’s $16,800/year or $453,600 lifetime. Boomers got Medicare negotiation. Millennials/Gen Z got neither. Generational wealth inequality + healthcare system inequality = young people literally rationing life-saving drugs.
In March 2026, Washington University researchers found that stopping GLP-1s, even briefly, erases cardiovascular benefits. Patients who stopped semaglutide or tirzepatide experienced immediate risk elevation for heart attack, stroke, and death.
Implication: GLP-1s aren’t one-off weight-loss treatment. They’re lifelong medications. Missing a month due to cost can have fatal consequences.
For uninsured and underinsured patients, this means: Can’t afford this month’s dose → skip it → cardiovascular benefits erase → higher risk of heart attack/stroke → system says it’s “their fault” for not having insurance.
Truth: System failed to price medication affordably. System created unaffordable medication. System blames patients when they ration.
Pharmaceutical companies argue: Real R&D cost is $5–15 billion per drug. Only high prices recoup. Risk is real — 90% of candidates fail; profitable drugs fund failed research. Competition drives innovation. Price controls stifle it. U.S. high prices subsidize lower-price markets.
Valid points: R&D is expensive. Pharma did need profit to fund GLP-1 development.
But: Once R&D is sunk, high prices serve pure profit. Novo Nordisk cut 35–50% without cutting innovation. Patent monopolies are government-granted; government can regulate them. Real solution: faster generic entry, cap copays at $50, fund R&D via public/nonprofit research.
Q: Can I get GLP-1 cheaper without insurance? A: TrumpRx (~$350/month), Mark Cuban Cost Plus Drugs, GoodRx, Roman offer $200–$500/month. Starter doses only. Quality/oversight varies. Talk to doctor.
Q: Will my insurance cover GLP-1? A: Most cover if diagnosed with type 2 diabetes or obesity (BMI >30). Weight loss (vanity) typically not covered. Prior authorization required (2–4 week wait). Ask your doctor to file appeals if denied.
Q: Is Medicare price ($245) permanent? A: Yes, for 2026. Subject to annual CMS review. Likely to remain low given political pressure and generics coming 2025–2027.
Q: When will generics be available? A: Semaglutide (Ozempic/Wegovy) generic 2025–2026. Tirzepatide (Mounjaro/Zepbound) generic 2028–2030. Generic prices will be $50–$150/month.
Q: Can I stop taking GLP-1s? A: No, if you want cardiovascular benefits. WashU 2026 study shows stopping even briefly erases heart protection. Lifelong drug for most.
Q: Do GLP-1s have side effects? A: Yes. GI side effects (nausea, constipation) affect ~30%. Rare but serious: pancreatitis, gastroparesis. Congress investigating safety Apr 2, 2026. Always discuss with doctor.
GLP-1 Pricing & Costs (Feb–Apr 2026): Novo Nordisk press release (Feb 24, 2026), CNBC (Feb 24, 2026), GLP-1 Journal/GLP-1 Health (Jan 2026), AARP/Harvard Gazette/STAT News (2026).
Medicare Negotiation: White House fact sheet (Nov 2025), KFF, Healthcare.gov.
Generational Impact: Business Insider (Apr 2024), Harvard Gazette (Feb 2026), Washington University Medicine (Mar 2026).
Congress Investigation: Bloomberg Government News (Apr 2, 2026), Senate Health Committee.