Breaking News
Popular News






Enter your email address below and subscribe to our newsletter

The mental health crisis in America is not a mystery and it is not an accident. 23.4% of U.S. adults — 61.5 million people — experienced mental illness in 2024. Nearly half of Gen Z always or often feel anxious. The youth suicide rate surged 57% between 2009 and 2019. And the mental health system that was supposed to catch these people? It was deliberately defunded over four decades of bipartisan policy failure, leaving gig workers, graduates, and young families with nowhere to turn except a medical debt crisis waiting to happen.

Key Takeaways:
• 23.4% of U.S. adults experienced mental illness in 2024 — 61.5 million people
• Youth suicide rates surged 57% from 2009 to 2019
• Reagan’s 1981 budget cut repealed Carter’s Mental Health Systems Act, eliminating community mental health funding
• The 2008 Mental Health Parity Act has been ignored by insurers for 16 years with minimal enforcement
• Mental health claims are denied 85% more often than standard medical claims
• 122 million Americans live in federally designated mental health professional shortage areas
• Average therapy session costs $143–$200 without insurance — Millennials earning median wages cannot afford weekly care
• By 2037, the U.S. will be short 31,000 psychiatrists

The numbers aren’t alarming — they’re catastrophic. According to the National Alliance on Mental Illness, 23.4% of U.S. adults experienced mental illness in 2024. That’s 61.5 million people. Of those, 14.6 million experienced serious mental illness — conditions severe enough to significantly limit daily functioning.
For younger generations, the data is even grimmer. A 2023 Gallup survey found that nearly half — 47% — of Gen Zers aged 12–26 often or always feel anxious. A separate Harmon Healthcare IT study found that 61% of Gen Zers have received a formal medical diagnosis for anxiety. One in four Gen Z adults reported more bad days than good in the past month. Millennials, meanwhile, are statistically the generation most likely to die from drugs, alcohol, and suicide combined.
The suicide data hits differently. The overall U.S. suicide rate rose nearly 40% since 2000. Among youth ages 10–24, the rate surged 57% between 2009 and 2019 — a span that includes the peak smartphone adoption years — and continued climbing. In 2021, there were 48,183 suicides in the U.S., reversing a two-year decline. Among 15–24 year-old males, the rate reached 17.9 per 100,000.
These aren’t background statistics. They’re the exhaust fumes of a system that was engineered — through decades of deliberate policy choices — to fail anyone who couldn’t afford to pay out of pocket.

To understand why mental health care is so inaccessible today, you have to go back to 1963. President Kennedy signed the Community Mental Health Act, which set in motion a shift from large psychiatric institutions toward community-based care. The idea was sound: close the warehousing hospitals, replace them with local mental health centers embedded in communities, give people real treatment instead of indefinite institutionalization.
The problem was the money never followed. States began releasing patients from hospitals. The community mental health centers were chronically underfunded from the start. And then came 1981.
President Jimmy Carter had tried to fix this with the Mental Health Systems Act of 1980 — landmark legislation designed to properly fund community mental health infrastructure, expand access, and create national coordination. It passed. It had broad support. It never went into effect. Ronald Reagan was elected in November 1980, and by August 1981, his Omnibus Budget Reconciliation Act had repealed most of it.
What replaced it was a block grant — a lump sum handed to states with minimal federal oversight and a built-in funding cut. Federal mental health spending was slashed roughly 25% in Reagan’s first term. States, facing their own budget pressures, spent the money on lower-priority populations rather than the severely mentally ill. The community centers that were supposed to replace institutions never got the resources to operate at scale.
California is the instructive case study. Before Reagan — who as governor signed the Lanterman-Petris-Short Act in 1967, accelerating deinstitutionalization — California’s state hospital census was 21,966. By the time he left the governorship in 1975, it had dropped to 6,431. The money saved from closing those beds was promised to community care. It largely went elsewhere. Today, 38.2% of California’s 92,000 prison inmates have a diagnosed mental illness. The state built a new kind of psychiatric institution — it just called it the criminal justice system.
This is the same generation that cut the social safety net while accumulating the largest share of American wealth in history. The mental health system didn’t collapse by accident. It was defunded by design, and younger generations have been paying the psychological price ever since.
In 2008, Congress passed the Mental Health Parity and Addiction Equity Act (MHPAEA). The law was simple in theory: health insurers cannot impose more restrictive coverage rules on mental health and substance use disorders than they do on physical medical conditions. No higher copays. No tighter prior authorization requirements. No stricter limits on visits.
It has been, by virtually every measure, a spectacular failure of enforcement.
Researchers reviewing the law’s first 16 years found “flat rejection of mental health parity” by insurers, with enforcement hampered by three systemic failures: inconsistent interagency coordination between state insurance regulators and mental health agencies; extreme policy complexity (especially around “nonquantitative treatment limitations” — think prior authorization criteria that are technically compliant but functionally exclusionary); and a near-total absence of political will to actually penalize violations.
The numbers tell the story. According to NAMI data:
Wait — those look like higher in-network rates for mental health. They are. And yet mental health claims are still denied 85% more often than standard medical claims. The mechanism is in the invisible fine print: non-quantitative limitations. Insurers approve you being “in network” but then deny specific sessions, impose stricter prior authorization criteria, and use medical necessity standards that are applied more aggressively to mental health than to physical conditions. It’s parity on paper, denial in practice.
The result: 1 in 5 mental health claims are denied outright. The out-of-pocket burden for those who pursue care despite denials is staggering — averaging $117 per visit in high-cost-sharing situations, compared to $38 for those with better coverage. The ACA subsidy cliff compounds this for anyone who falls off marketplace coverage, leaving them entirely uninsured for mental health at precisely the moment financial stress peaks.

Even if you could afford care and your insurance would actually pay for it, there’s still the small matter of finding a provider who’s accepting patients, takes your insurance, and has an opening before 2027.
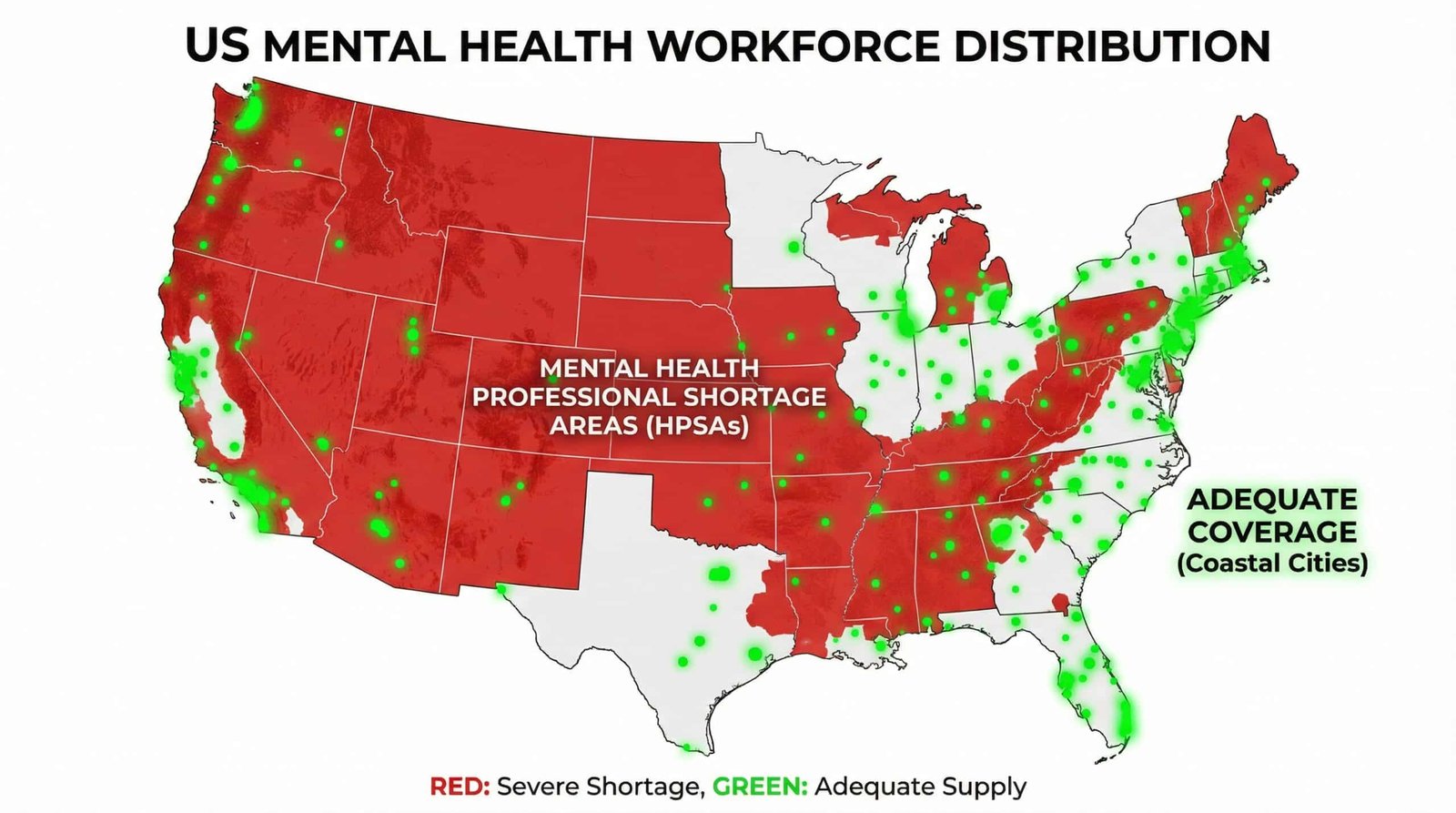
According to the Kaiser Family Foundation, 47% of the U.S. population in 2022 lived in a mental health workforce shortage area. AAMC data puts the current estimated shortage at 14,280 to 31,081 psychiatrists. The National Council for Mental Wellbeing projects that by 2037, the shortage will widen further as demand continues to outpace the pipeline of new providers.
As of 2021, 129.6 million Americans lived in one of the 5,930 federally designated Mental Health Professional Shortage Areas (HPSAs). That’s not a rural-only problem — HPSAs exist in urban cores too, concentrated in low-income and uninsured communities where Medicaid cuts have driven providers out of the market entirely.
Over half of U.S. counties have zero psychiatrists. For a Millennial living in rural Ohio or a Gen Z worker in suburban Georgia, getting a psychiatric evaluation might mean a 3–6 month wait, a 90-minute drive, and cash out of pocket because the nearest psychiatrist stopped taking new insurance patients years ago. The Medicaid reimbursement rates are, on average, 40% lower than cash-pay rates — which is why providers don’t take it. Fifty-one percent of U.S. counties have no psychiatrists at all.
The workforce shortage is itself a downstream consequence of the defunding era. When mental health centers were shuttered and insurance reimbursements were slashed, psychiatry and psychology became economically unattractive for new graduates drowning in medical school debt. Why go into a field where insurance won’t pay you, patients can’t afford you, and the regulatory environment is a compliance nightmare? The pipeline dried up before the demand even started rising.

Let’s talk numbers. Without insurance, the average therapy session in the U.S. costs $143.26, according to a 2024 analysis of more than 143,000 providers. In practice, it ranges from $100 to $350 per hour depending on location, provider type, and specialty. For a Millennial or Gen Z worker earning the national median wage of approximately $56,000 per year — take-home roughly $3,800 per month — a weekly therapy session at $150 costs $600 per month. That’s 16% of take-home pay. On top of rent, student loans, and prescription drug costs.
The out-of-pocket cost for out-of-network mental health care is even steeper. JAMA Network data shows cost-sharing for out-of-network behavioral health is significantly higher than for chronic physical conditions — the same insurance plans that cap your out-of-network orthopedic bill at 30% may leave you with 50–60% of a psychiatric hospitalization. For the lowest-income quartile of Americans, this is not a choice. It is a wall.
The alternatives — community mental health centers, federally qualified health centers, sliding-scale clinics — exist but are severely overburdened. Wait times of 3–6 months for an intake appointment are standard at most low-cost community providers. Medicare’s mental health coverage only covers 80% of approved costs after the Part B deductible, and finding a provider who accepts Medicare assignment for mental health is an adventure in itself.
The gap between what younger Americans need and what they can access is not a market failure in the traditional sense. It is the entirely predictable outcome of a policy trajectory that began in 1981 and has never been seriously reversed.
The dominant media narrative blames smartphones and social media for the youth mental health crisis. Jonathan Haidt’s The Anxious Generation made the case memorably and sold millions of copies. The thesis is not wrong — social media has measurable correlations with anxiety, depression, and body image issues, particularly for adolescent girls.
But it is radically incomplete — and it is politically convenient for the people responsible for the actual structural failures.
Consider: Millennials — who came of age largely before the smartphone era — show the same catastrophic mental health indicators as Gen Z. Millennials are the most likely generation to die from the combined causes of drugs, alcohol, and suicide. Their peak anxiety and depression years predate Instagram. The gig economy trap eliminated the employer-sponsored insurance that would have covered mental health care. Student loan debt created a chronic financial stressor that began before the iPhone existed. The housing crisis priced them out of stability. These are structural economic conditions, not screen-time problems.
A peer-reviewed generational analysis published in 2025 found a 20.7% overall prevalence of anxiety symptoms and 17.4% of depression symptoms — with no significant gender differences in Generation Z. Anxiety is not a gendered social media phenomenon. It is a generational economic one.
The social media argument also conveniently deflects from the fact that no politician who defunded community mental health centers, voted against parity enforcement, or gutted Medicaid reimbursement rates has ever faced meaningful accountability for it. It is much easier to blame Mark Zuckerberg than to explain why the Mental Health Systems Act was repealed six months after it passed.
Mental health care is expensive because decades of policy failures created a system with too few providers, inadequate insurance coverage, and no cost controls. Reagan’s 1981 repeal of the Mental Health Systems Act eliminated community mental health funding. Insurer noncompliance with the 2008 Mental Health Parity Act has never been seriously enforced. The result is a market where demand vastly outstrips supply, and the people who need care most are the least able to pay for it.
Millennials are statistically the most at-risk generation for “deaths of despair” — deaths from drugs, alcohol, and suicide combined. They came of age during the 2008 financial crisis with record student debt, entered a gig economy that stripped employer-sponsored insurance, and now face a housing market that prices them out of stability. Each of these economic stressors directly correlates with mental health deterioration, and the mental health system they need was gutted before most of them were born.
The Mental Health Parity and Addiction Equity Act (MHPAEA), signed in 2008, requires insurers to cover mental health conditions on equal footing with physical medical conditions. It has been routinely violated for 16 years with minimal enforcement. Insurers exploit vague “nonquantitative treatment limitations” — prior authorization criteria, medical necessity standards — that are applied more aggressively to mental health than physical health. Mental health claims are still denied 85% more often than standard medical claims.
As of 2021, 129.6 million Americans — nearly 40% of the country — lived in one of 5,930 federally designated Mental Health Professional Shortage Areas. By 2037, HRSA projects a shortage of up to 31,081 psychiatrists. Over 51% of U.S. counties have zero psychiatrists at all, meaning most of rural (and much of urban low-income) America has effectively no access to psychiatric care.
This article draws on federal datasets, peer-reviewed research, and independent policy analysis. Mental illness prevalence statistics from NAMI’s 2024 report. Gen Z anxiety data from a 2023 Gallup survey and Harmon Healthcare IT analysis. Suicide rate trends from the CDC MMWR and Annie E. Casey Foundation. Historical defunding timeline from the ALA’s DttP journal, GovTrack legislative records, and Capitol Weekly’s investigative reporting on the Lanterman-Petris-Short Act. Insurance parity enforcement gaps from NAMI’s “Out-of-Network, Out-of-Pocket, Out-of-Options” report (2024), PMC-published research on state-level MHPAEA enforcement, and STAT News coverage of insurer resistance to 2024 parity rule updates. Therapist shortage projections from AAMC, the National Council for Mental Wellbeing, and HRSA workforce projection fact sheets. Therapy cost data from SimplePractice’s 2023–2024 national rate survey and a 2024 multi-provider analysis. Out-of-pocket cost-sharing data from JAMA Network Open. Shortage area geography from KFF Mental Health Care HPSA state indicator data.